What Is Meningitis?
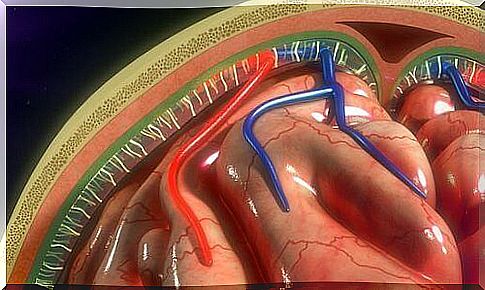
Meningitis is an inflammation of the membranes that cover the central nervous system. These membranes are called meninges or meninges. Because this causes abnormal inflammation in the body, this is a disease. The good news is that fortunately this disease is not currently a common disease.
Meningitis is normally caused by infectious organisms. The most common form is viral encephalitis. The bacterial meningitis, on the other hand, is more serious.
Meningitis can lead to brain damage. In extreme cases, this can also lead to death. That is why it is essential that you detect meningitis in time and treat it as soon as possible.
What are the meninges?
Imagine for a minute that your brain is like a fruit. This fruit contains a nut and juice inside. The juice travels through various points in the fruit to keep it in good condition.
Now suppose that the skin of the fruit is your skull. What’s under the shell, the nut, is our brain. These are soft, smooth and delicate. Under the skin, the outermost layer of the fruit, there are three other layers. So the moisture circulates through all these layers to preserve the fruit.
These three layers under our skull are the meninges. They are three membranes that cover and protect our brain and spine. The brain and spine together make up our central nervous system.
It is important to remember that the brain and spine are the most protected organs in our body. The meninges will not only absorb and absorb blows, but will also act as a filter to prevent dangerous microorganisms from entering our central nervous system. Meanwhile, cerebrospinal fluid circulates through our brain membranes. This moisture also has protective and immunity functions.
Where is meningitis most common?
Meningitis is a common epidemic on the African continent, especially in the Sub-Saharan region during the dry season. The epidemics in that area last anywhere from two to three years. After all, they alternate with periods of rain. Unfortunately, the lack of medical care leads to high death rates in the population. The worst meningitis epidemic in the region was in 1996, when more than 25,000 people died.
In Western countries, only three out of every 100,000 people are victims of bacterial meningitis. The virus only occurs in ten cases out of every 100,000.
Risk Factors
- Dry season
- Children
- Infectious diseases
- Immunosuppression
- intoxication
Causes of meningitis
Meningitis is normally a result of another infection. Usually this is a virus. However, cases of non-infectious causes have been reported.
Virus
- Enterovirus
- Herpes simplex virus
- HIV
- West Nile virus (spread through mosquitoes)
bacteria
Depending on the age of the individual, there are different infection risks caused by a number of microorganisms.
- Newborns under three months
- Group-B Streptococci
- E Colic
- Children older than three months
- meningococci
- pneumococci
- Haemophilus Influenzae
- Adults
- meningococci
- pneumococci
- Listeria monocytogenes
How does the disease manifest itself?
The micro-organisms enter the meninges through the bloodstream, directly or indirectly.
The bacteria that are harmless in the nose, mouth and pharynx enter the bloodstream. They then pass through the barrier between the blood and the brain in the areas that are most vulnerable.
In this way, the bacteria also reach the cerebrospinal fluid of the subarachnoid space. It is there that they finally cause the infection in the meninges.
The other modes of transmission are direct, such as skull fractures, operational intervention and so on. In addition, the bacteria can also enter through zones such as the paranasal sinuses.
Symptoms
- Fever, especially in children and newborns
- Trembling and shivers
- Dizziness and vomiting
- light shyness
- Stiff neck
- convulsions
- headaches
- Decreased level of consciousness
The illness comes on suddenly, with fever, headache, dizziness and vomiting. In children, however, the symptoms may be less obvious. For example, drowsiness, like irritability, can also be symptoms.
brain damage
Cerebral edema is an injury often caused by inflammation. This causes increased skull pressure, making it difficult for blood to reach the brain.
It follows that the brain does not get enough oxygen, so the brain cells begin to die. In some cases, brain damage can also be fatal. This is especially the case when meningitis is not treated.
Diagnosing meningitis
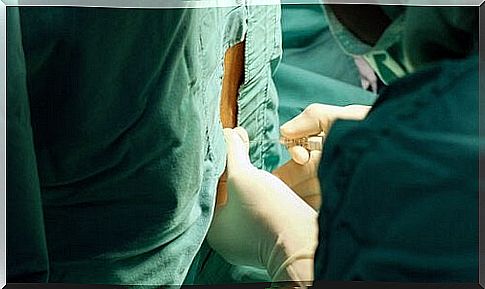
The suspicion of meningitis is always clinical. However, an exact diagnosis is obtained through a puncture in the lumbar region.
With such a lumbar puncture one extracts cerebrospinal fluid from the intervertebral discs. To do this, the doctors insert a long needle into the back.
Types of meningitis
Meningitis can have a viral cause or a bacterial cause, depending on the cause of the infection.
- The viral meningitis has a mild prognosis and requires no treatment.
- The bacterial meningitis, on the other hand, is very serious and requires hospitalization for treatment. The chances of death are very high, even with the correct treatment.
You can also classify the disease according to the stage of the disease, namely acute, subacute or chronic. However, these criteria are not used very often.
Therapy
The patient should be given antivirals and antibiotics as soon as possible.
To reduce the risk of inflammation and brain edema, doctors will prescribe corticosteroids such as dexamethasone. This will reduce the risk of brain damage.
In addition, there are also some general methods that can help you with acute infections, such as drinking a lot, keeping your fever under control and so on.
Timely treatment will thus greatly reduce the long-term risk, as well as the risk of death.
Possible consequences
- Deafness
- Epilepsy
- Cognitive disorders
- hydrocephalus
- Passing away
Newborns and adults have between a 20 and 30 percent chance that the disease will be fatal. This risk then decreases to two percent in older children.
Appearance
Currently, research is underway into a means to preventively vaccinate children against meningitis. However, this vaccine is optional and can be used after the child’s second month of life.
In case of symptoms, do not hesitate to consult your doctor about this.